Services
EARLY DIAGNOSIS AND EARLY TREATMENT ARE KEY TO CONTROLLING DISEASE AND MAINTAINING TEETH FOR A LIFETIME.
Periodontal Disease Therapy
Mouth-Body Connection
Did you know that the health of your mouth could be affecting the health of the rest of your body? Are you aware that by treating diseases of the mouth, the overall health care costs for diabetics is lower? Have you heard that poor oral health can lead to a greater risk of developing heart disease? If you were unaware of any of this, please read on.
Over the last several years, the medical and dental communities have been discovering that they are more closely related than once thought. The unifier appears to be chronic inflammation, which is the body’s response to an infection or irritant. It has now been shown by both communities that poor oral health (chronic inflammation) is linked with poor overall health of the body.
Periodontal (gum) disease is a chronic inflammatory disease in the mouth which, according to the American Academy of Periodontology, has been shown to be linked to the following health conditions:
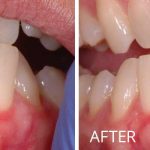
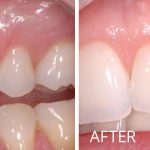
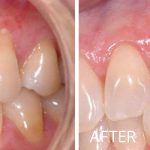
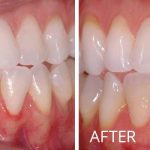
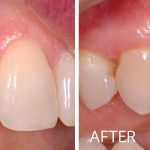
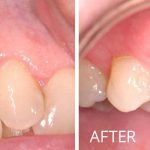
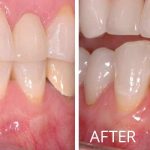
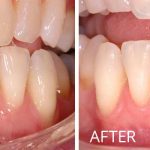
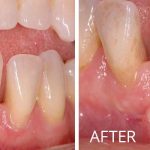
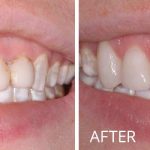
Soft Tissue Grafting
Do you have sensitivity in your mouth when you drink cold beverages? Do you notice the teeth in your mouth are appearing longer? Are you concerned with dark spots along the gum line showing in your smile? If “Yes!”, then soft tissue (gum) grafting may be the procedure you need.
Frenectomy
Esthetic Periodontal Procedures
Are you unhappy with the appearance of your smile?
Do you show too much gum tissue when you smile?
Are you concerned about the appearance of dark
root surfaces or long teeth in your mouth?
If you answered “Yes!” to any of these questions, Esthetic Periodontal Procedures may be right for you.
Some periodontal procedures are designed to greatly enhance a patient’s esthetics. These procedures can be performed alone, or in conjunction with restorative procedures, to produce a more pleasing appearance to the patient. Esthetic procedures can help…
A patient who is concerned with the appearance of his or her teeth looking too short
A patient who has concerns with the gumminess of his or her smile
A patient’s gum line is that uneven
A patient who has darkened root surfaces which cause cosmetic concerns
Dental Implants
Are you currently missing a tooth? Do you have a removable appliance that moves around in your mouth? Would you like a new, strong set of teeth that are secure and do not need to be removed? If you answered “Yes!” to any of these questions, dental implants may be a solution for you to improve your life.
Implant Site Preparation
When a tooth is removed from the mouth, the supporting bone starts to break down. If an implant is the accepted next step in the treatment plan, then a procedure called socket preservation can be performed at the time the tooth is removed. This will maintain the supporting bone structure until the implant is placed. Going without a tooth or implant for a long period of time can result in a substantial loss of the supporting bone.
Occasionally, bone loss is such that there is not enough bone into which a dental implant can be successfully placed. In these situations, additional procedures (bone grafting) may be required to regenerate sufficient bone structure into which a dental implant could then be placed.
Sedation
The Advanced Periodotics & Implants team understands that some people can experience apprehension or anxiety when at the dentist. We do all that we can to make our patients as comfortable as possible during their procedures. In order to accomplish this goal, we offer relaxing medications for use before and during the procedures.
You, the patient, will have maximum input regarding your experience during a procedure. Some people choose to have only local anesthesia (Novocaine) and be fully aware during surgery. Many people, however, feel uncomfortable with this and prefer Nitrous Oxide, Oral, or IV sedation as to be less aware or not aware of the activities of surgical procedures. Our providers can help you choose the option that will make your experience as comfortable as possible. Please review our different sedation options available below to determine which best would accommodate your needs.